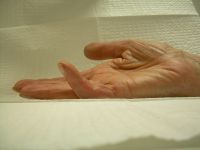
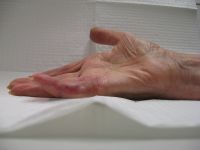
The treatment of Dupuytren's contracture bounded by factual constraints of its biology:
- There is not a pharmacological cure.
- Open surgery has significant risk of permanent complications, even for experienced surgeons.
- Recurrence is common after surgery.
- More radical surgery results in longer remission, but proportionally higher rates of complications.
- Open
surgery for recurrent Dupuytren's contracture has twice the
complication rate of first time surgery, and recurrences may not be
able to be treated with repeat surgery.
- PIP
contractures recurring after fasciectomy usually
involve issues independent of Dupuytren's such as flexor
sheath shortening and PIP capsuloligamentous contractures.
- Recurrent
PIP contractures occuring in the absence of clinical Dupuytren's
disease generally do not progress after the first postoperative year.
In addition, there are personal observations that:
- isolated small
finger PIP contractures in women are so prone to rapid recurrence that
dermofasciectomy should be considered as the first open procedure.
- PIP
fusion is a safer alternative to repeat palmar procedures for recurrent
PIP contractures, but may require significant (1-2 cm) shortening.
This
case is presented to demonstrate some of the difficulties encountered
in the treatment of recurrent Dupuytren's contracture. |